

Island Health, which has been looking after patients since 1894, is weeks away from opening Guernsey's newest primary care centre.
The multimillion-pound, two-storey redevelopment at L'Aumone, immediately to the west of the existing surgery, will triple the space for patients and staff and equip the Practice to meet modern expectations of primary care.
Though the current surgery was purpose built nearly 50 years ago, the march of time has caught up with it: consultation rooms are small, the space for pharmacists and secretaries smaller still.

Pictured: The current GP surgery and pharmacy at L'Aumone.
"Patients and staff have been very tolerant with us for a long time," says Dr Robbie Hanna, the partner in the Practice who is leading the redevelopment.
It suited a time when GPs provided more acute care, seeing patients once with short-term, self-limiting illnesses. There has since been a shift to more chronic or long-term care – obesity, mental ill health, diabetes, therapy.
This, in turn, says Dr Hanna, "lends itself less to the idea of an old-style GP prescribing penicillin and more to a health centre with a wider range of services".
The new surgery is 11,000 square feet with room for further expansion – larger than the surgery at Grandes Maisons Road in St. Sampson's which, along with one in Town, makes up the Island Health Practice.
It will house 12 large consulting rooms, some designed for minor operations and physical therapies; spacious reception and waiting rooms; clerical offices, rest rooms and an educational space upstairs; bariatric space; and better technology. There will be more parking for all forms of transport.

Pictured: Dr Robbie Hanna in front of the new surgery, which is due to open before the end of the year.
"Patients and staff are excited by the prospect of fit-for-purpose facilities and a wider range of services," says Dr Hanna.
"We have listened to their ideas and concerns. Medicine is changing. Patients are being supported to manage and improve their own health in purpose-built health hubs. There is more chronic disease management in primary care.
"There are more preventative activities going on and social prescribing is becoming commonplace, which is brilliant, helping people with loneliness and chronic low mood and people who have lost their connection with fitness.
"Obesity and poor mental health are two great epidemics of the modern age. For younger people, communication is changing. We do a lot more telephone consultations now and more tele-medicine. You need technology to do that and we're limited in the current premises.
"We look forward to extending our musculoskeletal and sports medicine services, augmented by our ultrasonography services. Early detection of cardiovascular conditions and aneurysms will continue in improved surroundings, allowing for more specialised equipment. Dermatology services will be extended to provide mole mapping and more skin cancer surgery.
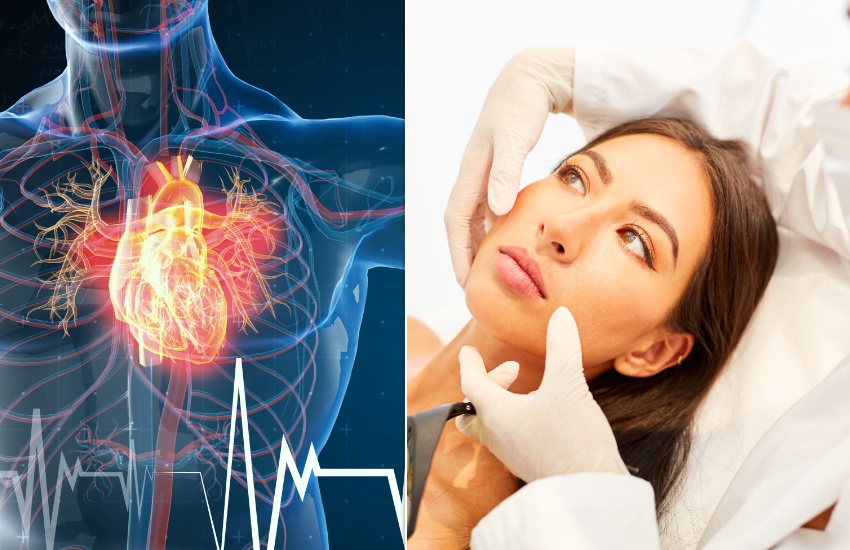
Pictured: Island Health expects its new surgery at L'Aumone to assist in delivering modern primary care medicine, including early detection of cardiovascular disease and a range of dermatology services.
"We hope now to have the space to engage more and share our resources with our colleagues in the third sector. Traditionally, we have often been looking at the wrong end of the telescope, treating the effects of ill health, and the need in the future is to do more work at the other end to prevent ill health, but that requires more space and more services than we have in the current surgery."
Initially, the pharmacy at L'Aumone will move into three rooms in the new building while the existing surgery is refurbished to house an expanded pharmacy, including a pharmacy consultation room, and possibly a new paramedical service yet to be confirmed.
"The pharmacy building is struggling because it, too, was built for another age. Pharmacology and the pharmacy are more complex now and have a central role providing advice to patients. We are talking about extremely capable professionals who know everything there is to know about medication, so we want to look after them and encourage them and put them at the heart of our team."

Pictured: Dr Hanna said that Island Health has wanted to develop a new surgery at L'Aumone for many years. The Practice is weeks away from realising its objective.
Dr Hanna acknowledges that the Practice would ideally have redeveloped and expanded years ago.
"Even in the mid- to late-90s, we could see that space was an issue, and that the level and range of our services were restricted by this building. And we could see from the template at St. Sampson's how well that worked for patients and staff."
Land was purchased around the original surgery, but for a long time States' planning policies prevented its development.
The partners examined other sites, such as the Castel and King Edward Hospitals, but found the purchase and decant costs prohibitive. Then, in 2016, the States' Island Development Plan "rezoned the land next door and opened it up for development".
The partners shook hands with their contractor, R G Falla, in December 2019, weeks before the first outbreak of covid-19, "but the timetable is delayed only by four weeks – you have to take your hat off to the professionals running the construction project".

Pictured: The Practice considered moving to other sites, such as the Castel Hospital, before securing permission to build a new surgery at L'Aumone immediately to the west of the existing surgery.
In the mid- to late-90s, Dr Hanna was in his 30s, not long arrived in Guernsey from Belfast: two communities which could hardly have been more different.
"My father was born into a Presbyterian Protestant family. My mum was Catholic. They met just after the war. Looking back on it, though at the time I wasn't thankful for it, I think being exposed to the two faces of Northern Ireland was a real advantage."
He was born in Dublin, in the Republic, and moved with his family to Belfast, in the north of the island, when he was barely a year old. The period known as 'The Troubles' began before he left primary school.
"There was really societal breakdown. The whole of civil society and its institutions, which we tend to take very for granted here, was really holding on by its fingertips. Society became very polarised. I think it wasn't a very happy time for my parents, but as a child you kind of accept how it is. To be searched or for a bomb to go off or to hear gun fire at school wasn't an unusual occurrence."

Pictured: A girl running in West Belfast at the location of a flashpoint during 'The Troubles'. Dr Hanna was born in Dublin but grew up in Belfast during some of the city's most difficult years.
"I qualified at Queen's [University, Belfast] in 1983 and spent seven years in the NHS in Northern Ireland. It's a fantastic place; the people are brilliant; I loved it." Dr Hanna and his wife married in 1990 and there was the question of where to build their lives and potentially start a family.
"I had a contact here – a guy called John Curran. I was at school with John and in the Scouts with him. He was the year above me. He told me Guernsey was fantastic and we moved here, initially in the Vale, and it was a very happy time.
"We've had four children here. It's been an extremely welcoming place. I can't speak highly enough of Guernsey. It's a meritocracy – nobody wanted to know your background or what your relationship was with anyone – entirely different to what I was used to. It's only when I looked back over my shoulder that I fully appreciated what a divided society Northern Ireland was. Obviously, we had to leave our families, and that was a wrench, but we try to stay in touch and get back when we can."
General Practice was a different world when Dr Hanna arrived in Guernsey. He remembers working from a former surgery in St. Sampson's, slightly west along Grandes Maisons Road from the present surgery.

Pictured: The new surgery at L'Aumone is even larger than the surgery at Grandes Maisons Road, which is also part of the Island Health Practice.
"That was really old school. I'd be sat here seeing my patient and there was a hatch which would open up and they'd pass the notes in. When I started, some patients would come in to see me – I was 30 years old, full of enthusiasm but a bit green – and they would keep standing and wait for me to invite them to sit down.
"I was told there was a doctor – not in our practice, I might add – who had a sign on his desk: one patient, one problem, one consultation. My average consultation now is 12 to 15 minutes and patients often want to discuss more than one issue.
"In those days, most GPs had come from the UK whereas a lot of our younger doctors today have a link with Guernsey. Of course, a great development is that there are now many more women doctors. I've seen society change a great deal in the 32 years I've been here. I'd like to think that we've tried to change with it."
Dr Hanna now shares his patients with Dr Abigail Griffiths, a GP with special interests in diabetes, adolescent health and learning disability.
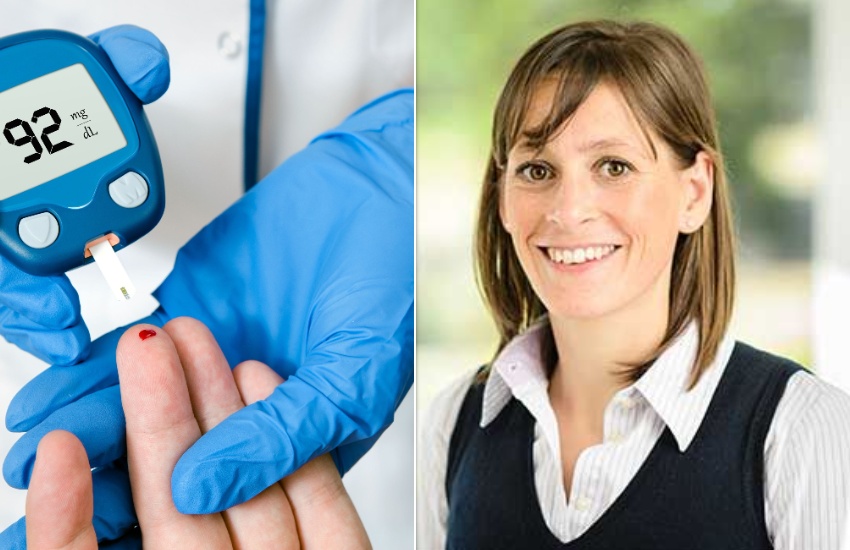
Pictured: Dr Hanna shares his practice with Dr Abigail Griffiths, whose special areas of interest include diabetes. Credit: Island Health.
Dr Hanna talking of 'his' "list of patients" leads our conversation onto the model of primary care locally, in particular the loyalty between a patient and his or her doctor and the concept of the family doctor, which has endured in Guernsey long after weakening in many other places.
"Yes, the family GP, who is there at least most of the time when you need him or her. I think people in Guernsey appreciate that.
"Traditionally, there hasn't been much movement of patients between one practice and another. I think a lot of it is tradition – where your mum or dad went – and this enduring relationship with your GP. Someone who has been there when you were a child and sees your children being born and growing up.
"It is an absolute joy for a GP to see generations of the same family and go through their life journey with them. The joys of having kids, the tribulations of an illness, standing by them as they're going through difficult times in life.

Pictured: Dr Hanna is now among the island's longest-serving GPs.
"I don't know about you, but when anyone in my family is ill, that to me is the worst time in life. You're looking to someone who is reliable, dependable, compassionate, good counsel, someone who is there at times of joy and times of huge crisis – that's the GP.
"We often break bad news, which is difficult, but I ask myself: Who is the best person to tell a patient about an unpleasant diagnosis? It's probably the GP with whom you have an enduring relationship. Yes, that can be traumatic, but it is a privilege, too.
"There’s a lot of debate about our model of primary care. I think there is benefit in having skilled, experienced people seeing a patient at the outset when he or she first presents. Sometimes a less skilled or experienced person would refer more because they are uncertain.
"That is an important role in acute care – that experienced, skilled judgement about who needs to be referred and who doesn't. You don’t want everyone with acid reflux having to see a gastroenterologist or everyone with a nosebleed having to see an ear, nose and throat specialist. We've got to protect secondary care for the people who really need it.

Pictured: One of the important roles of primary care is to act as the 'gatekeeper' of referrals to secondary care.
"But GP care is certainly changing with a big focus on chronic care: people with long-term diabetes, heart conditions, enduring mental health challenges, and taking them back from secondary care and looking after them on an ongoing basis.
"In that sense, I think the future will involve GPs taking on more complexity in patient care. Accessibility is also important in our model. Being able to see a doctor the same day shouldn't be taken for granted – in a lot of places in the world, including the UK, that's nearly unheard of.
"I think our model helps recruitment. We've got some younger partners. In Guernsey, they are able to develop special interests and have more autonomy and are more involved with their own practice. The NHS is in a constant state of reorganisation whereas we tend to have a bit more stability as well as all the stakeholders being closer together.
"Ongoing education for GPs is really important now. It's all about retaining good staff – you educate them, you remunerate them, you look after them and you give them a good working environment. We don't have all of that at the moment in our existing premises. We have these discussions with people sat on the edge of desks. So that's another reason to look forward to our move next door."

Pictured: Dr Hanna on the roof of the new surgery development at L'Aumone, which has space for further expansion in the years ahead should that prove necessary.
The wait has been long and not without complications and setbacks, but the ambition of Dr Hanna and his partners is within touching distance.
Barring any unforeseen, last-minute obstacles, their new surgery will open by the end of November, transforming experiences for their patients and colleagues.
This interview was first published in the current edition of CONNECT magazine, Express' sister publication.
The online version of CONNECT magazine can be read HERE.
Credit for pictures of Dr Hanna: Paul Chambers.
CONNECT interview: Meet the custodian of our island's heritage
CONNECT interview: The man behind the scenes at the KGV
FOCUS: A Life in Light and Darkness
FOCUS: Work-life balance is next challenge for PR expert
Comments
Comments on this story express the views of the commentator only, not Bailiwick Publishing. We are unable to guarantee the accuracy of any of those comments.